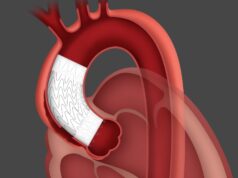
Collaboration between cardiothoracic and vascular surgeons is key to achieving success in aortic arch interventions, a session at CX 2020 LIVE has concluded. Speakers presenting in a session entitled Aortic Arch Consensus and Stroke from Thoracic Endovascular Procedures (STEP) underlined the benefits of consultation between disciplines to achieve the best outcomes for patients.
 Aortic arch interventions are among the most technically challenging of reconstructive surgeries, requiring exceptional skills and dexterity. Through presentations, discussion, and polling, the session—chaired by Roger Greenhalgh (London, UK) and moderated by Stéphan Haulon (Le Plessis-Robinson, France)—aimed to tackle some vital questions, including how to reduce the risk of stroke in thoracic aortic endovascular procedures, what the best options are for the left subclavian branch, and how best to approach aortic arch aneurysms.
Aortic arch interventions are among the most technically challenging of reconstructive surgeries, requiring exceptional skills and dexterity. Through presentations, discussion, and polling, the session—chaired by Roger Greenhalgh (London, UK) and moderated by Stéphan Haulon (Le Plessis-Robinson, France)—aimed to tackle some vital questions, including how to reduce the risk of stroke in thoracic aortic endovascular procedures, what the best options are for the left subclavian branch, and how best to approach aortic arch aneurysms.
Roberto Chiesa (Milan, Italy) provided a comprehensive overview of total endovascular, hybrid, open and frozen elephant trunk repair techniques in aortic arch aneurysms, looking at which is the best strategy to use in different scenarios, and the European Society for Vascular Surgery (ESVS) recommendations for each. He stressed: “The clever surgeon chooses the best option for the patient.”
A key message that emerged was the need for multidisciplinary decision-making. Chiesa revealed that, at his centre, meetings take place every day between cardiothoracic and vascular surgeons to decide on the choice of technique. His message also illustrated the potential that exists for using patient characteristics to choose between endovascular and open reconstruction. “It depends on the extent of the disease and the situation of the patient. In a fit patient, also in a young patient … open surgery can represent a good option. Endovascular repair offers possibilities that open surgery cannot offer,” he said.
“Acceptable results in fit patients” can also be achieved using the Frozen Elephant Trunk technique, said Chiesa, describing a hybrid strategy—a combination of both open and endovascular technique—as “a good option in high to moderate-risk patients”, and total endovascular branch repair as providing improving results in anatomically suitable patients. He closed his presentation with the prediction: “I think that will represent the future.”
Kevin Mani (Uppsala, Sweden) echoed Chiesa’s comments on the need for consultation with cardiothoracic colleagues when he discussed the feasibility of endovascular arch repair for type A dissection. He explained that more than two-thirds of post type A dissection repair patients are technically eligible for endovascular arch repair. He said: “It is not an easy procedure for the surgeon or the patient, so everybody is happy if it can be done endovascularly at the second stage.”
He concluded: “More than two-thirds of post type A dissection repair patients are technically eligible for endovascular arch repair. Future advancements that may increase this number include a greater awareness among cardiovascular surgeons of a sufficient ascending graft length.
Chiesa’s colleague, Luca Bertoglio (Milan, Italy), also presented an edited case of a carotid subclavian bypass. He explained that left subclavian artery (LSA) revascularisation is recommended in aortic procedures to reduce the incidence of spinal cord ischaemia and stroke. Bertoglio noted this was the procedure that “we prefer to perform in our centre”.
 He outlined how the carotid subclavian bypass is performed, and dealt with common difficulties encountered, including the impact of anatomy on the choice of implant. A lively discussion followed his presentation, at the end of which Greenhalgh declared himself to have “been extremely entertained”.
He outlined how the carotid subclavian bypass is performed, and dealt with common difficulties encountered, including the impact of anatomy on the choice of implant. A lively discussion followed his presentation, at the end of which Greenhalgh declared himself to have “been extremely entertained”.
Gustavo Oderich (Rochester, USA) outlined preliminary experience with a range of device options that would enable the LSA to stay patent. He began with the statistic that “30–60% of thoracic endovascular aortic repair [TEVAR] patients require Zone 2 incorporation with coverage of the LSA”. Considering the implications, he detailed: “We know LSA coverage without revascularisation is associated with more arm ischaemia, posterior circulation events, and spinal cord injury”.
He noted that patient-specific fenestrated stent grafts have been available for over two decades, and added that reports from the Cleveland Clinic and the Hamburg group demonstrate that mortality and stroke can be an issue, particularly if there is misalignment of the stent graft requiring arch manipulations.
Oderich considered the options for left subclavian branch incorporation, and concluded: “Zone 2 extension is needed in up to 60% of TEVAR patients, and the preliminary experience with LSA branch devices indicates low morbidity and stroke rates, with high patency rates”.
In the discussion following his presentation, a participant from Moldova asked Oderich, “In what subgroup of patients would either a bypass or transposition be used rather than a branch endograft?” to which Oderich responded that the “obvious” cases would be when the subclavian artery is not suitable for a branch.
Oderich noted that, given the investigational nature of some grafts, surgeons are still “shying away” from treating patients with certain indications, for example a very dominant vertebral artery. That being said, “with increased experience, as we showed, the patency rate is excellent”. He was positive looking forward: “I do think there will be a benefit of a branch over a bypass”.
Polling conducted during the session revealed that 85% of the audience would alter reconstruction in the arch according to underlying pathology, and when asked to consider the statement “Open is best,” 63% disagreed.