 Stefan Verheye (Antwerp Cardiovascular Centere ZNA Middelheim, Interventional Cardiology, Antwerp, Belgium) and others report in JACC: Cardiovascular Interventions that the use of a sirolimus-coated balloon (Virtue, Caliber Therapeutics) to treat in-stent restenosis in patients with a bare metal stent/drug-eluting stent is associated with “excellent” procedural outcomes and a similar rate of late lumen loss as existing non-stent in-stent restenosis options.
Stefan Verheye (Antwerp Cardiovascular Centere ZNA Middelheim, Interventional Cardiology, Antwerp, Belgium) and others report in JACC: Cardiovascular Interventions that the use of a sirolimus-coated balloon (Virtue, Caliber Therapeutics) to treat in-stent restenosis in patients with a bare metal stent/drug-eluting stent is associated with “excellent” procedural outcomes and a similar rate of late lumen loss as existing non-stent in-stent restenosis options.
The authors report that although drug-eluting stents are seen as the gold standard approach for treating in-stent restenosis, they have limitations because they result in “additional metal layers and polymers that reduce vessel flexibility, promote geometric distortion and lumen deterioration (especially small vessels) and generally limit the viability of subsequent stenting”. Verheye et al add that angioplasty with a paclitaxel-coated balloon is another “feasible treatment option” but “challenges to this technology remain”, including that the drug paclitaxel “is widely considered to be less effective and more toxic than other antirestenotic drugs”—such as sirolimus and its analogues.
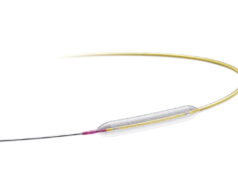
The aim of the present study was to evaluate the feasibility of Virtue to treat in-stent restenosis. According to Verheye et al, the balloon combines “the promising approach of encapsulation of sirolimus in submicron particles with angioplasty without a balloon coating”. “Instead, a liquid formulation is delivered thorough precise micropores in the balloon, concurrently with angioplasty,” they write.
In the first-in-human study, 50 patients with in-stent restenosis (following either a drug-eluting stent or bare metal stent) underwent coronary angioplasty with the Virtue balloon. The primary safety endpoint was the 30-day rate of target lesion failure—a composite of cardiac death, target vessel myocardial infarction, and clinically-driven target lesion revascularisation—and the primary performance endpoint was in-stent late lumen loss at six months.
Results
Verheye et al comment: “No target lesion failures were reported through the 30-day follow-up for the entire 50 patient study population. Among the 49 intention-to-treat patients at the six month follow-up, one underwent coronary artery bypass and four received target lesion revascularisation for a target lesion failure rate of 8.2% and major adverse cardiac event rate of 10.2%.” They add that in-segment late lumen loss was 0.31±0.52mm “which met the established criteria for superiority to historical plain balloon angioplasty values (p<0.001)”.
The authors write that, based on these results, the use of a microporous balloon to deliver sirolimus nanoparticles to the vessel wall was both feasible and safe, noting that the device “may represent a new approach to the treatment of in-stent restenosis”. They conclude: “The acceptable quantitative coronary and composite clinical outcomes for the Virtue angioplasty balloon in a challenging patient population warrant further evaluation in appropriately powered clinical trials.”
Verheye told Cardiovascular News: “The promising results of the SABRE trial demonstrate the potential for effective treatment of in-stent restenosis with the Virtue sirolimus eluting balloon. This novel stent-free therapeutic device represents an important innovation in coronary interventions and I look forward to confirmation of these results in a well-powered clinical trial.”