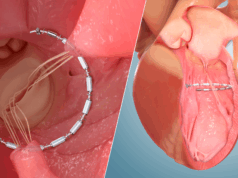
The placement of an interarterial shunt device—the Corvia atrial shunt (Corvia Medical)—did not reduce the total rate of heart failure events in a population of patients with heart failure with preserved or mildly reduced ejection fraction (HFpEF or HFmrEF).
This was the conclusion of REDUCE LAP-HF II, a randomised, multicentre, sham-controlled trial. Primary results from the trial, which investigated the safety and efficacy of the Corvia device in the prespecified patient population, were presented at the Technology and Heart Failure Therapeutics conference (THT 2022; 1–2 February, New York, USA, and virtual) and published online in The Lancet.
Sanjiv Shah (Northwestern University Feinberg School of Medicine, Chicago, USA) and Martin Leon (Columbia University Irving Medical Center, New York, USA) served as lead principal investigators of the trial which was performed in 89 healthcare centres across the USA, Canada, Europe, Australia and Japan. Results were presented at THT by Shah.
In their reporting of the trial results in The Lancet, Shah, Leon et al detail that patients were eligible for inclusion in the trial if aged ≥40 years, had symptomatic heart failure, an ejection fraction of at least 40%, and pulmonary capillary wedge pressure during exercise of at least 25mmHg while exceeding right atrial pressure by at least 5mmHg.
The trial’s primary endpoint was a hierarchical composite of cardiovascular death or non-fatal ischaemic stroke at 12 months, the rate of total heart failure events up to 24 months, and change in Kansas City Cardiomyopathy Questionnaire (KCCQ) overall summary score at 12 months. Prespecified subgroup analyses were conducted for the heart failure event endpoint.
In their Lancet paper the study team reports that a total of 1,072 participants were enrolled in the trial, of whom 626 were randomly assigned to either the atrial shunt device (n=314) or sham procedure (n=312). There were no differences between groups in the primary composite endpoint (win ratio 1 [95% CI 0·8–1·2]; p=0·85) or in the individual components of the primary endpoint, the study team reports, and no differences in the composite safety endpoint between the two groups (n=116 [38%] for shunt device vs. n=97 [31%] for sham procedure; p=0·11).
The prespecified subgroups demonstrating a differential effect of atrial shunt device treatment on heart failure events were pulmonary artery systolic pressure at 20W of exercise, right atrial volume index, and sex, Shah, Leon et al note.
Results of the study led investigators to conclude that placement of an atrial shunt device did not reduce the total rate of heart failure events or improve health status in the overall population of patients with heart failure and ejection fraction of greater than or equal to 40%.
While the overall outcome of the trial found no reduction in total rate of heart failure events, a press release from Corvia—issued following the presentation of the results—focused on patients with normal exercise pulmonary vascular resistance (PVR) and without a pacemaker, which the company says may represent a responder group that derives significant clinical benefit from the treatment.
“In this first-of-its-kind device trial for a complex and heterogenous type of heart failure, we have identified a large potential responder population with meaningful clinical benefit. The ability to predict responders and non-responders is groundbreaking and has significantly advanced our understanding of the role of atrial shunting in HFpEF,” Shah was quoted as saying in the release.
According to Corvia, the subanalysis showed that patients with normal exercise PVR, indicating the absence of pulmonary vascular disease (PVD), and without a pacemaker, derived significant clinical benefit, including a reduction in heart failure events compared to sham (0.12 vs. 0.22 events per patient-year, p=0.007) and a significant and clinically meaningful difference in health status improvement over sham (+5.5 points) as assessed by the Kansas City Cardiomyopathy Questionnaire (KCCQ) overall summary score.
“Clinical trials in patients with HFpEF have been challenging to date given the heterogeneous nature of the HFpEF syndrome,” Shah told Cardiovascular News. “In the REDUCE LAP-HF II trial, we show that exercise invasive haemodynamic phenotyping of patients, which allows for the gold standard diagnosis of the HFpEF syndrome, also provides insight into underlying disease biology (responsiveness of the pulmonary vasculature to increased blood flow via placement of the interatrial shunt) and identifies a potential responder group for this therapy. Although confirmatory studies are required, our trial moves us one step closer to a future of precision medicine therapeutics in HFpEF.”