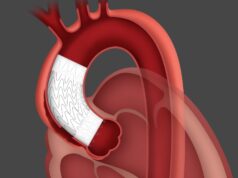
Gore has announced positive results from the REDUCE study, which is assessing the safety and efficacy of its septal occluder devices for the percutaneous closure of patent foramen ovale (PFO). The data were presented at the European Stroke Organisation Conference (ESOC; 16–18 May, Prague, Czech Republic).
The controlled, open-label REDUCE study assessed the efficacy and safety of PFO closure using Gore septal occluder devices in 664 randomised patients—aged 18 to 59 with a history of cryptogenic stroke—across 63 investigational sites in seven countries. The trial met its primary endpoint by showing a statistically significant, 76.6% (p=0.001), reduction in recurrent ischaemic stroke in patients that underwent PFO closure in conjunction with antiplatelet therapy versus those who underwent antiplatelet therapy alone after an average of 3.4 years follow-up.
In addition to the primary endpoint of reduction of recurrent stroke, the study also met its co-primary endpoint of reduction of new brain infarct, inclusive of silent brain infarct, through PFO closure. An increased risk of clinical stroke, dementia, and cognitive dysfunction has been associated with silent brain infarct. This marks the first time a study assessed the relationship between PFO closure and reduction of new brain infarct. Patients underwent baseline and two-year follow-up MRI scans to determine if new brain infarct occurred. New brain infarct was patients, yielding a 49.6% (p=0.024) relative risk reduction for PFO closure on new brain infarct.
Furthermore, the data showed no difference in the patient-based rate of serious adverse events between test and control groups. Device- and procedure-related serious adverse events occurred in 1.4% and 2.5%, respectively, of test patients. Patients experienced low rates of bleeding, deep vein thrombosis, and pulmonary embolism, with no significant difference between test and control groups. There was a significantly higher rate of serious atrial fibrillation in the test group (2.3% vs. 0.4%) but the majority of atrial fibrillation was peri-procedural (80% had onset within 30 days of the closure procedure) and had rapid resolution (70% with resolution within two days of onset).
Scott Kasner (Perelman School of Medicine, University of Pennsylvania, USA), US neurology national principal investigator for the REDUCE study, says: “The REDUCE data is ground-breaking for patients who have suffered a cryptogenic stroke attributed to a PFO. Until now, there has never been a study of a PFO closure device that showed statistically significant reduction in stroke recurrence in the primary intent-to-treat analysis. Other PFO closure device trials had to rely on secondary analysis, including following patients for up to a decade, before achieving statistical significance. Also of note is the level of safety the Gore Cardioform septal occluder demonstrated, with no significant difference shown in the rate of serious adverse events between patients implanted with the device and those in the control arm. This trial demonstrates noteworthy verification that PFO closure with the Gore Cardioform septal occluder is a valuable procedure to reduce recurrent stroke and brain infarct when utilized in an appropriate patient population.”