
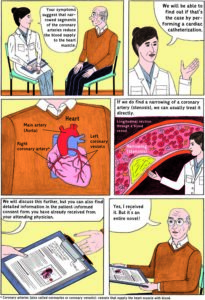
A pilot study, published as a research letter in the Annals of Internal Medicine, has found that patients who received comics or “medical graphic narratives”, as well as standard informed consent protocols (official consent form and a conversation with a physician), had greater comprehension of the coronary angiography procedure that they underwent and less anxiety than those who only received the standard protocols.
Writing in the Annals of Internal Medicine, Anna Brand (Charité – Universitätsmedizin Berlin and DZHK, Berlin, Germany) and colleagues report that the 2018 European guidelines for myocardial revascularisation highlighted the need for “active patient participation and the use of terminology that the patient understands”. However, they add that prior studies have indicated that “a large proportion of patients undergoing coronary interventions do not seem to understand the rationale for treatment and have erroneous perceptions regarded expected benefits”.
According to the authors, comic narratives “may communicate complex health information more clearly” than current approaches to explaining the necessary information. They state that comic-based approaches “allow each patient to acquire and process information at his or her own speed”, adding that “the use of pictures in close juxtaposition with written or spoken text has been reported to increase patients’ ability to understand and recall health information compared with text alone”.
In the study, 121 patients being considered for coronary angiography were randomised to receive standard informed consent protocols (61) or standard protocols plus comics (60). The primary outcomes were understanding of the procedure-related information and periprocedural state anxiety.
Brand et al found that patients who received the comics “had significantly better comprehension, which was attributable to higher scores in all three subcategories of comprehension items: procedural details, risks, and behavioural measures after procedure”. They also found that after the procedure, periprocedural state anxiety—as assessed by the Spielberger State-Trait Anxiety Inventory—was decreased in patients in the comic group but was increased in patients in the standard protocol alone group compared with their respective baseline levels. Furthermore, significantly more patients in the comics group felt that they were “well prepared” for cardiac catheterisation: 71.7% vs. 41% for the standard protocols alone group (p=0.01).
“Our pilot trial provides novel proof-of-concept data regarding the benefit of medical graphic narratives as supplementary patient information and consent material before coronary angiography,” Brand et al observe. They add that larger, multicentre trials are warranted to further assess the advantage of a comic-assisted informed consent approach.
Brand told Cardiovascular News: “In this context, the adage ‘a picture is worth a thousand words’ has proven to be very useful to assist and improve the patient informed consent procedure. More than 93% of the patients completely denied feelings of being not taken seriously by the comic, underlying the high acceptance of this new method (high percentage of patients had university or a polytechnic degree). Most of the patients gave a very positive feedback and welcomed the new informed consent approach.”










