This advertorial is sponsored by Pi-Cardia
As more transcatheter aortic valve implantation (TAVI) procedures are performed in lower-risk patients, there is an increasing focus on the long-term lifespan of the bioprosthetic valve—with a recognition that for a younger cohort of patients there may be a greater potential need for repeat procedures due to valve degeneration over time.

Leaflex (Pi-Cardia) is a novel, non-implant device that could defer the need for TAVI in younger patients who may require multiple valve implants in their lifetime, or potentially even prevent the need altogether for TAVI in some patients. Further to this, Leaflex could act as a possible alternative to balloon valvuloplasty in patients who may be deemed too old or frail for TAVI, or to improve TAVI outcomes in heavily calcified and bicuspid aortic valves. Cardiovascular News speaks to Eberhard Grube (University Hospital, Bonn, Germany) about the potential for the device to “change the way we think about aortic stenosis” and the next steps for study of the procedure.
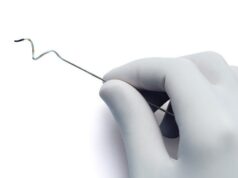
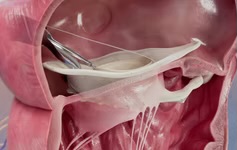
“You could say that this is a next-generation aortic valve repair device, or maybe you can say that it is an alternative aortic valve repair device,” Grube describes. Leaflex is a transfemoral transcatheter device that uses two mechanical structures for scoring aortic valve calcification. This consists of a proprietary Expander, which is positioned into the left ventricular outflow tract and lifts the aortic leaflets into contact with the frame, three scoring arms positioned in the aortic root. “Basically, it modifies the motion of the leaflets, by a controlled application of force—scoring the calcification within the leaflets without embolisation of the calcium particles,” Grube explains. This has the advantage of allowing the valve leaflets to move more easily, be more pliable, and open up the area of flow, he adds.
During the Leaflex procedure, a deflectable transfemoral delivery catheter is inserted via a 16Fr sheath, delivered and positioned into the aortic root using fluoroscopic guidance. Mechanical expansion of the device scores calcification within the leaflets, and rotation of the arms allows scoring to be performed at different targeted sections of each aortic valve leaflet. Scoring lines create separation between the calcium deposits on the two sides of the scoring line, in order to regain leaflets’ flexibility, allow their mobility, and improve valve haemodynamics.
“When this particular force is applied to the calcified leaflets, it scores from the aortic side, but the ventricular side of the leaflets remain basically intact, which is obviously very important because you would like to preserve the integrity of the leaflet so that the patient does not end up with aortic insufficiency,” says Grube.
First-in-human study of Leaflex was completed across six European centres and has demonstrated the functionality and safety of the device, as well as its potential to have a significant effect on aortic valve area among aortic stenosis patients. Grube comments that the initial results show that the device can improve flow access across the valve, increase the mobility of valve leaflets and increase the opening area of the aortic valve without damaging the leaflets. He notes: “So far the application in humans both during surgery and TAVI , the device has proved to be very safe, and very efficacious as far as gradients and aortic opening areas are concerned.”
Clinical study
Further clinical studies have commenced to evaluate the acute and long-term results following treatment with Leaflex as a standalone procedure. Grube believes that this will be important in establishing exactly which scenarios and in which patients the device is best suited. He sees the procedure as having a particular potential in younger patients—where although there has been an increase in the number of TAVI procedures performed in recent years, questions still remain over the long term—although a benefit could also be seen in older patients, or those for whom a TAVI procedure is not feasible. There is further potential, Grube comments, for the device to be deployed in regions where there is limited access to TAVI, or where the lack of reimbursement for a TAVI procedure means it is out of reach for much of the population.
 “There is an ongoing discussion, and a very important discussion, on the present TAVI platforms, [about] the lifetime management for aortic stenosis patient” says Grube. “Do we start with surgery or do we start with TAVI—given our present experience that bioprosthetic valves might degenerate within a ten year timeframe.”
“There is an ongoing discussion, and a very important discussion, on the present TAVI platforms, [about] the lifetime management for aortic stenosis patient” says Grube. “Do we start with surgery or do we start with TAVI—given our present experience that bioprosthetic valves might degenerate within a ten year timeframe.”
This leads to questions about how best to treat a patient aged 65 years or younger, he comments, who potentially could require two implants over the remainder of their lifetime. This is where he sees the greatest opportunity for Leaflex. “If we apply the Leaflex in these patients we might defer the need for TAVI over the next few years and then start the discussion, which is a lot different in their outcomes than beginning at 65,” Grube says.
On the need for robust data, he adds: “It is very important that we can demonstrate with this device, not only feasibility but particularly the sustainable results of scoring the calcium, improving the opening area and the flow through the aortic valve. I think this is interesting and I hope we have those results in the near future. Then we will see how the debate will change.”
Grube suggests that if further study of the device can demonstrate its efficacy, Leaflex will be of great interest to the interventional cardiology community as an option for the treatment of aortic stenosis. “The first thing that we have to look into as physicians is what we are doing for our patients,” he says. “That is something that definitely carries weight and I think that once the device is more broadly known, and we have more results, then we will think differently about how to approach aortic stenosis—I am convinced about that. Whether we call it a game changer remains to be seen, but it will definitely change the landscape of our platforms for treating this disease.”