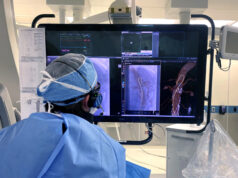
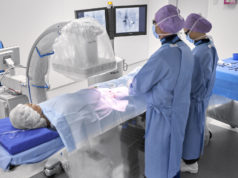
Ryan D Madder (Frederik Meijer Heart and Vascular Institute, Spectrum Health, Grand Rapids, USA) and others write in Circulation: Cardiovascular Interventions that increased body mass index (BMI) among patients undergoing cardiac catheterisation is associated with a significant increase in physician radiation dose. They add that further studies are needed to determine whether patient obesity might have adverse effects for physicians in the form of increased radiation exposure during coronary angiography.
Madder et al comment that increased BMI is known to increase radiation exposure to patients undergoing coronary angiography. They add that, in theory, increased BMI could also lead to increased radiation exposure to physicians, explaining that greater radiation doses are required to produce adequate images on obese images and this leads to greater amounts of scatter radiation. “The greatest source of physician radiation exposure during cardiac catheterisation comes from scatter radiation emitted from the patient,” the authors note. However, according to Madder et al, the impact of the patient BMI on radiation exposure to physicians is less well understand as its impact on radiation exposure to patients. Therefore, the aim of the study was to “evaluate the association of patient BMI and physician radiation dose during coronary angiography”
Using data from the SHIELD study, the authors identified 1,119 consecutive cases of coronary angiography. Of these, patient radiation dose information was available for 1,116 cases and physician radiation dose information were available for 1,114 cases. Real-time radiation exposure data were collected with a bedside monitor capable of displaying real-time radiation doses (RaySafe i2, Unfors RaySafe). Overall, based on BMI measurements, 83% of patients in the study were either overweight or obese. Furthermore, 50.1% were categorised as obese and 9.6% were categorised as morbidly obese.
The median radiation dose per case for physicians was 0.6. Madder et al report: “A significant increase in physician radiation dose was observed across increasing patient BMI categories. A patient BMI ≥40 was associated with a 7-fold increase in physician radiation dose compared with a patient BMI <25 (p<0.001).” However, the increase in exposure did differ depending on the procedure—a BMI ≥40 was associated with a 5-fold increase in physician exposure for patients undergoing coronary angiography but was associated with a 23.5-fold increase for patients undergoing percutaneous coronary intervention.
The authors state that their findings are “consistent with the concept that higher patient radiation doses, which were also observed to increase in a stepwise fashion with patient BMI result in a higher amounts of scatter radiation, the primary source of radiation exposure to physicians performing cardiac catheterisation”. They add that the findings are “concerning” because long-term radiation exposure among interventional cardiologists has been linked to “multiple adverse health effects”.
Furthermore, Madder et al note that increased BMI increased radiation exposure to physicians to a greater degree than it did for patients (7-fold vs. 2.1-fold). While they say that these results should be interpreted with caution, they state that physician radiation dose may increase out of proportion to dose area product. “For instance, it is possible that patient body habitus, particularly among morbidly obese patients, may prevent optimal positioning of accessory lead shields in some cases,” Madder et al comment.
They conclude: “Additional studies are needed to determine whether patient obesity may have adverse health effects on physicians as well, in the form of increased radiation doses during coronary angiography.”
Madder told Cardiovascular News: “It has been established that patient obesity results in a multiple of adverse health problems for patients. Our findings raise concern that patient obesity could also be adversely impacting the health of physicians in the cath lab, in the form of increased occupational radiation doses. These findings are concerning considering that prior studies have linked physician radiation exposure in the cath lab to the development of premature cataracts, early carotid atherosclerosis and vascular ageing, and possibly to an increased risk of left sided brain malignancies. I am hopeful that our study will lead to additional studies aimed to optimise radiation safety for both physicians and patients in the midst of the obesity epidemic.”